A Simple And Efficient Method For Radiolabeling Of Preformed Liposomes Y. Cao and M. R. Suresh, Faculty of Pharmacy and Pharmaceutical Sciences,University of Alberta, Edmonton, Alberta, Canada T6G 2N8 Abbreviations: CH, cholesterol; DISIDA, diisopropyl iminodiacetic acid; DSPE, distearoyl-phosphatidylethanolamine; FBS, fetal bovine serum; HSPC, hydrogenated soy phosphatidylcholine; HMPAO, hexamethylpropyleneamine oxime; PE, phosphatidylethanolamine; PEG, polyethylene glycol. Abstract A simple and efficient method for radiolabeling preformed liposomes was developed using hepatobiliary imaging agent 99mTc-diisopropyl iminodiacetic acid (99mTc-DISIDA). Chloroform extraction of 99mTc-DISIDA from aqueous solutions results in 80% radioactivity in the organic phase due to its lipophilic properties. However, with the presence of reduced glutathione (g -Glu-Cys-Gly), chloroform extraction results in only 30% of label in the organic phase because the 99mTc-DISIDA complex undergoes reduction decomposition to more hydrophilic species by reaction with glutathione. The incorporation efficiency of the 99mTc-DISIDA into the liposomes containing reduced glutathione was greater than 90%. The labeled liposomes were stable up to 24 h in saline and 90% FBS after preparation. Biodistribution studies in mice showed that 99mTc labeled liposomes accumulated in liver and spleen at 24 h postinjection, unlike 99mTc-DISIDA. Compared to hexamethylpropyleneamine oxime (HMPAO), the 99mTc-DISIDA compound is much cheaper and has a longer shelf life when used for liposome labeling. The labeling technique described here could be used for monitoring pharmacokinetic and pharmacodynamic changes of liposomes, and tumor or infection imaging when coupled with targeting antibodies. Introduction Liposomes are artificial lipoid systems consisting of one or more phospholipid bilayers arranged concentrically with aqueous compartments and a core. They are made predominantly from naturally-occurring phospholipid, therefore, they are biodegradable, nontoxic and do not elicit an immune response. Liposomes were first introduced in the early 1960s by the British scientist Alec Bangham (1). They have been employed as excellent models of biological membranes and very useful carriers of both lipid-soluble and water-soluble drugs due to their biodegradability, ease of preparation, and non-toxicity (2, 3). In recent years, the applications of these lipid spheres have been extended to enhance the drug efficacy and potency (4-6), reduce toxicities of encapsulated drugs (7-9) and target specific tissue sites (10). In scintigraphic studies, liposomes, which can carry radionuclides within the aqueous space, have potential diagnostic imaging applications (11). Gamma-emitting radionuclides, such as 99mTc,111In and 67Ga, have been encapsulated in liposomes for use as imaging agents (12-17). Some clinical trials for tumor imaging have already been started using labeled liposomes (18-20). Generally, two methods have been used to label liposomes for diagnostic imaging purposes. One involves the entrapment of radionuclides during the hydration of the lipids with the aqueous phase (14, 21). However, low encapsulation efficiency and batch production variability are two disadvantages of this approach. The second method is the labeling of preformed liposomes (18, 22). Labeling of preformed liposomes with radionuclides is ideally suited for clinical imaging applications wherein the liposomes can be formulated and distributed to the clinician as an unlabelled kit. This preparation is subsequently labeled on site with a short half-life radionuclide prior to clinical use. In this report, we describe the utility of the hepatobiliary imaging agent 99mTc-DISIDA with lipophilic properties (23, 24) to label preformed liposomes that contain reduced glutathione, and determine their biodistribution in mice. Materials And Methods Liposome Preparation The hydrogenated soy phosphatidylcholine (HSPC), cholesterol and phospholipid distearoyl-phosphatidylethanolamine (DSPE) were gifts from the Department of Pharmacology, University of Alberta. The liposomes were prepared using the method described previously (25). HSPC : Cholesterol (molar ratio 2:1) were mixed and dissolved in organic solvent chloroform to create a homogeneous mixture. The mixture was placed in a round-bottom flask and the solvent was removed under negative pressure using a rotary evaporator. An evenly-distributed thin lipid film was formed on the flask wall and stored in vacuo overnight. The thin lipid film was rehydrated with 50 mM reduced glutathione (g -Glu-Cys-Gly, Sigma, St Louis, Mo.) to produce multilamellar liposomes (MLV). Care was taken to disperse all of the dried lipid from the wall of the flask. The homogeneously sized liposomes were obtained by extrusion (Lipex Biomembranes Extruder, Vancouver, BC. Canada) through polycarbonate membrane filters successively with 0.2, 0.1 and 0.08 m m pore size until the average size distribution was ~100 nm in diameter. Removal of unencapsulated material was accomplished by ultracentrifugation (22). The liposome size was monitored by dynamic light scattering with a Particle Analyzer (Brookhaven Instruments Corporation, Holtsville, NY.). The liposome suspensions were diluted 300 times with the buffer used in the formulation, then the sample was allowed to equilibrate for 15 min. at room temperature followed by the size measurement at 25 oC. The concentration of the liposomes was determined by phosphorus content after perchloric acid treatment (26). Labeling Procedures 99m Tc-DISIDA was purchased from the local Edmonton Radiopharmaceutical Center (ERC). The radiochemical purity was estimated by instant thin layer chromatography (ITLC) prior to use. 99mTc-DISIDA was incubated with glutathione encapsulated liposomes for 40 min. at room temperature. The labeled liposomes were separated from 99mTc-DISIDA by passage over a Sephadex G-25 column (1x15cm). Labeling efficiencies were checked by determining the activity before and after column separation of the 99mTc labeled liposomes using a dose calibrator.Chloroform Extraction The chloroform extraction was conducted with four different formulations: free 99mTc-DISIDA, 99mTc-DISIDA mixed with empty liposomes, 99mTc-DISIDA incubated with 50 mM glutathione for 40 min, and 99mTc-DISIDA incubated with glutathione loaded liposomes for 40 min. A 0.1 mL aliquot of different liposome formulation was added to 0.9 mL of saline in a 10 mL centrifuge tube, 1mL of chloroform was added to the sample and vortexed for 10 sec. The tube containing the mixture was centrifuged at 700 g for 5 min to separate the two phases. The lower layer (organic phase) was removed by using a glass syringe and transferred to a clean tube. The organic phase retained in the tube was washed with 1 mL of saline, vortexed, spun and separated from water phase as before. The washing step was repeated up to 3 times, retaining the organic phase each time. The final organic phase containing the total lipids of the sample was separated from water-soluble liposomal contents, and was counted using a Beckman 8000 gamma counter (27). Stability of 99mTc Labeled Liposomes (a) Gel filtration chromatography: 99mTc labeled liposomes were incubated in saline and 90% fetal bovine serum (FBS) at 370C for 24 h. A small sample of liposome was analyzed on a Sephadex G-25 column at different time points. The column was eluted with PBS and aliquots of the fractions were counted. A sample of 99mTc-DISIDA was also similarly analyzed to determine the difference in the separation profiles of the labeled compounds. (b) Dialysis: A small volume of labeled liposomes in saline and 90% FBS, was placed in a dialysis sac (pore size 60 kD) and dialyzed against 100 mL of 0.9% saline at 370C for 24 h. Aliquots from the dialysates were taken at each time point and the radioactivity counted. Biodistribution Studies Ten week-old BALB/c mice were used for the biodistribution studies. 99mTc labeled liposomes (0.4 m mol as phospholipid and 5 m Ci / 0.1 mL) and free 99mTc-DISIDA (5 m Ci / 0.1 mL) were injected into the tail vein of normal mice. At 24 h. postinjection, the BALB/c mice were anesthetized with Metofane and a blood sample was obtained by cardiac puncture prior to euthanasia. The organs were removed, thoroughly washed with saline, weighed and counted using a gamma counter. Biodistributions were calculated as percentage of the injected dose per gram and per organ. Total blood volume, bone, muscle, brain and skin mass were estimated as 7.3%, 10%, 40%, 0.7% and 13% of total body weight, respectively (28). Results And Discussion Radiolabeled liposomes have been successfully used to monitor pharmacodynamic changes of liposomes and image tumors, abscesses, ischemic and infarcted regions (15, 16, 17, 29, 30). 99m Tc is the best candidate for imaging studies due to its short half-life, pure photon emitter and suitable energy. Encapsulating 99mTc during the rehydration of the lipid film with aqueous phase has been used to label liposomes (14, 31). This method is not convenient for clinical purposes due to individually-made preparations instead of batch-production and low incorporation efficiency (about 20-30%). Further, 99mTc has been used to directly label preformed liposomes based on using stannous chloride as a reducing agent (32). Reduced 99mTc is added to the liposomes and bound to the liposome outer surface. This surface-labeling approach is technically simple and good for the production of the vesicles in a pharmaceutically acceptable form. However, the bound 99mTc dissociates rapidly from the liposome surface in vivo by exchanging with plasma protein and accumulates in the thyroid, stomach and kidney.The lipophilic compound HMPAO has
been successfully used to label preformed liposomes (22). This method
has high labeling efficiency and stability because HMPAO, as a lipophilic chelator, can
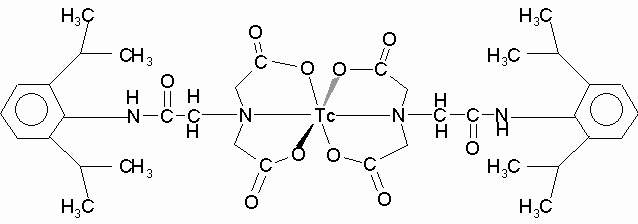
carry Efficient labeling of preformed liposomes was observed in our studies using 99mTc-DISIDA (Figure 1). 99mTc-labeled derivative of IDA (Iminodiacetic acid) was first introduced by Loberg et al. (33) for use as a hepatobiliary imaging agent. Later, IDA derivatives like 2,6-diethyl, p-ethoxy, and p-iodo-IDA were developed and all showed excellent hepatobiliary specificity while differing in blood clearance and urinary excretion (34). 99mTc DISIDA is a newer derivative and has been shown to have better hepatobiliary characteristics (23, 24).
The organic component of 99mTc-DISIDA is a bifunctional chelate having both the properties of technetium binding (iminodiacetic structure) and hepatobiliary processing (aromatic system). The lipophilic properties of this compound was demonstrated in chloroform extraction studies (Table 1) where more than 80% of the 99mTc-DISIDA was extracted into the organic phase from the aqueous phase with 99mTc-DISIDA alone or mixed with empty liposomes. The tripeptide (g -Glu-Cys-Gly) glutathione (MW 307.3 D) is involved in many aspects of metabolism, including removal of hydroperoxides, protection from ionizing radiation, maintenance of sulfhydryl status of proteins and aiding detoxification. Many of these functions are accomplished by reactions at the cysteinyl sulfhydryl group (35). When glutathione was incubated with 99mTc-DISIDA, the 99mTc complex might undergo decomposition by reduction with cysteinyl sulfhydryl group of glutathione to become more hydrophilic species. This resulted in only less than 30% of radioactivity being extracted into organic phase from aqueous phase (Table 1). This could also be an explanation for trapping of 99mTc inside of liposomes when glutathione was encapsulated in the inner aqueous phase of liposomes. Table 1. Chloroform Extraction of Radioactivity from Saline Phase.
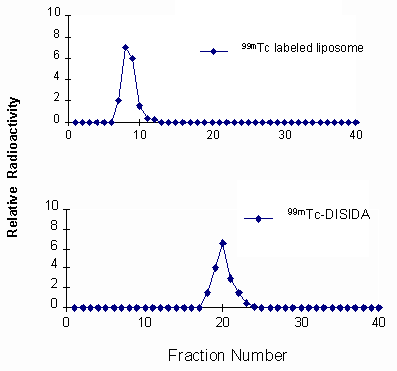
Values are expressed as mean ± standard deviation (n=4). Chromatography profile of the labeled liposomes on a Sephadex G-25 column shows that almost 90% of the radioactivity was recovered in the void volume associated with the liposome fraction (Figure 2). However, 99mTc-DISIDA alone eluted much later when chromatographed separately.
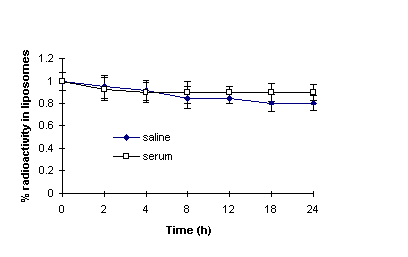
The stability of 99mTc labeled liposomes were demonstrated by both resolution of the labeled liposomes through the Sephadex G-25 column and dialysis against saline at various time points of post-labeling (Figure 3). Only about 15% and 20% of the radioactivity was released over 24 h when labeled liposomes were incubated with 90% FBS and saline respectively. The retention difference of the labeled liposomes incubated with serum and saline is probably due to the binding of radioisotope to serum components which could not diffuse through the dialysis membrane (32).
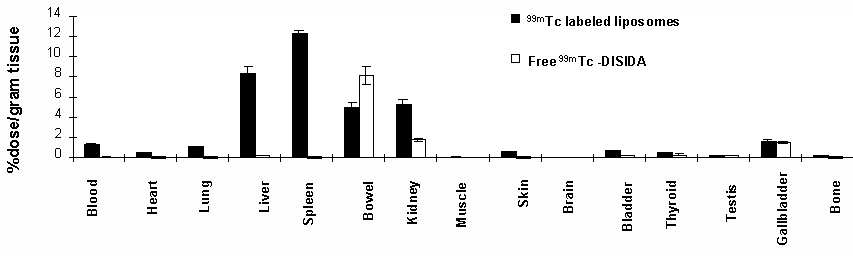
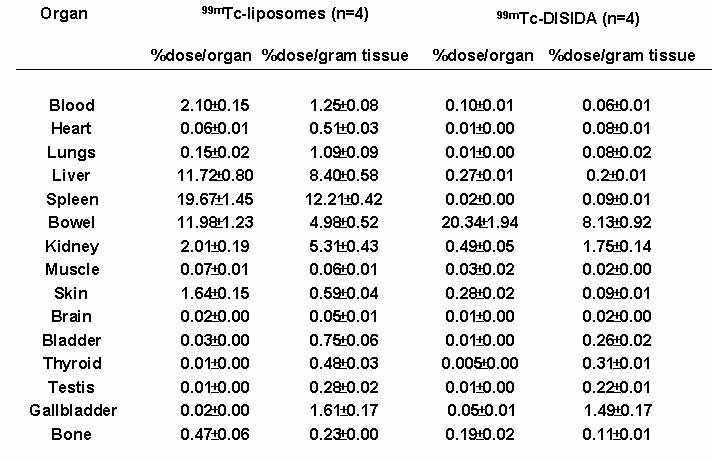
Biodistribution studies obtained from tissue samples at 24 h. post-injection of 99mTc labeled liposomes (Figure 4 and Table 2) show that significant radioactivity was localized in the liver and spleen (8.4% and 12.2% dose/gram, respectively, P<0.001) comparing with free 99mTc-DISIDA. This is because the liver and spleen are two major organs of the reticuloendothelial system (RES) which are known to accumulate and metabolize liposomes. However, 99mTc-DISIDA, used for imaging and functional studies of liver and bile, is processed by the hepatocytes within a few minutes after administration and excreted rapidly via the hepatobiliary system to the intestine (36). Therefore, after 24 h post-injection, there is much less radioactivity remaining in liver (0.2% dose/gram) and spleen (0.09% dose/gram). Significant difference was also found in the blood pool due to longer circulation time of liposomes compared to rapid excretion of free 99mTc-DISIDA. The conventional liposome formulations have a tendency to accumulate in the reticuloendothelial system and this has compromised their applications in drug delivery involving other tissues (37). Recently, liposomes exhibiting greatly prolonged blood retention were developed, by incorporating certain lipids, such as mono-sialo-ganglioside (GM1) or synthetic lipids derivatized with the hydrophilic polymer polyethylene glycol, into the liposomal membrane (38). Improved therapeutic effect was observed using the long-circulating liposomes (37, 39). For tumor imaging, long-circulating liposomes may be attractive candidates due to their high tumor accumulation (40). Thus, the methodology we described above could also be employed for labeling long-circulating liposome post-formulation of these vesicles. In conclusion, the labeling technique presented here shows a practical alternative for monitoring pharmacokinetic and pharmacodynamic changes of liposomes or liposomal derivatives, and could also be used for tumor or infection imaging, especially coupled with targeting antibodies. Figure 4. Biodistribution curve shows the difference of tissue uptake between 99mTc labeled liposomes and free 99mTc-DISDIA.
Table 2. Tissue Biodistribution of 99mTc Labeled Liposomes at 24 H Post-Injection
Data derived from mean ± standard deviation (n=4). Acknowledgments M.R.S. thanks MRC and Biomira for chair support, ACB and NSERC for grant funding. References Bangham, A. D., Standish, M. M. and Watkins, J. C. The action of steroids and streptolysin S on the permeability of phospholipid structures to cations. J Mol Biol 13: 138-144, 1965. Gregoriadis, G. and Florence, A. T. Liposomes in drug delivery. Drugs 45: 15-28, 1993. Kim, S. Liposomes as carriers for cancer chemotherapy: current status and future prospects. Drugs 46: 618-638, 1994. Mayer, L. D., Nayar, R., Thies, R. L., Boman, N. L., Cullis, P. R. and Bally, M. B. Identification of vesicle properties that enhance the antitumour activity of liposomal vincristine against murine L1210 leukemia. Cancer Chemother Pharmacol 33: 17-24, 1993. Mayer, L. D. and St.-Onge, G. Determination of free and liposome-associated doxorubicin and vincristine levels in plasma under equilibrium conditions employing ultrafiltration techniques. Anal Biochem 232: 149-57, 1995. Gabizon, A., Chemla, M., Tzemach, D., Horowitz, A. T. and Goren, D. Liposome longevity and stability in circulation: effects on the in vivo delivery to tumors and therapeutic efficacy of encapsulated anthracyclines. J Drug Target 3: 391-398, 1996. Bally, M. B., Masin, D., Nayar, R., Cullis, P. R. and Mayer, L. D. Transfer of liposomal drug carriers from the blood to the peritoneal cavity of normal and ascitic tumor-bearing mice. Cancer Chemother Pharmacol 34: 137-146, 1994. Rahman, A., Treat, J., Roe, J. K., Potkul, L. A. and Alvord, W.G. Phase I clinical trial and pharmacokinetic evaluation of liposomal encapsulated doxorubicin. J Clin Oncol 8: 1093-1100, 1990. Lim, H. J., Masin, D., Madden, T. D. and Bally, M. B. Influence of drug release characteristics on the therapeutic activity of liposomal mitoxantrone. J Pharmacol Exp Ther 281: 566-73, 1997. Loughrey, H. C., Ferraretto, A., Cannon, A. M., Acerbis, G., Sudati, F., Bottiroli, G., Masserini, M. and Soria, M. R. Characterization of biotinylated liposomes for in vivo targeting applications. FEBS Letters 332: 183-188, 1993. Lasic, D. Liposomes. American Sci 80: 20-31, 1992. Gregoriadis, G., Neerunjun, D. E. and Hunt, R. Attempts to improve localization in tumor tissues. Life Sci 21: 357-370, 1977. Richardson, V. J., Jeyasingh, K., Jewkes, R. F., Ryman, B. E. and Tattersall, M. H. N. Possible tumor localization of Tc-99m-labeled liposomes: effects of lipid composition, charge and liposome size. J Nucl Med 19: 1049-1054, 1978. Oku, N., Namba, Y., Takeda, A. and Okada, S. Tumor imaging with technetium-99m-DTPA encapsulated in RES-avoiding liposomes. Nucl Med Biol 20: 407-412, 1993. Tilcock, C., Ahkong, Q. F. and Fisher, D. Polymer-derivatized technetium 99mTc-labeled liposomal blood pool agents for nuclear medicine applications. Biochim Biophys Acta 1148: 77-84, 1993. Ogihara-Umeda, I., Sasaki, T., Toyama, H., Oda, K., Senda, M. and Nishigori, H. Rapid tumor imaging by active background reduction using biotin-bearing liposomes and avidin. Cancer Res 54: 463-467, 1994. Ogihara-Umeda, I., Sasaki, T., Kojima, S. and Nishigori, H. Optimal radiolabeled liposomes for tumor imaging. J Nucl Med 37: 326-332, 1996. Presant, C. A., Proffitt, R. T. and Turner, A. F. Successful imaging of human cancer with Indium-III labeled phospholipid vesicles. Cancer 62: 905-911, 1988. Presant, C. A., Blayney, D., Proffitt, R. T., Turner, A. F., Williams, L. E., Nadel, H. I., Kennedy, P., Wiseman, C., Gala, K. and Crossley, R. J. Preliminary report: imaging of Kaposi sarcoma and lymphoma in AIDS with indium-111-labelled liposomes. Lancet 335: 1307-1309, 1990. Kubo, A., Nakamura, K. and Sammiya, T. Indium-111-labeled liposomes: dosimetry and tumor detection in patients with cancer. Eur J Nucl Med 20: 107-113, 1993. McDougall, I. R., Dunnick, J. K., Goris, M. L. and Kriss, J. P. In vivo distribution of vesicles loaded with radiopharmaceuticals: a study of different routes of administration. J Nucl Med 16: 488-492, 1975. Phillips, W. T., Rudolph, A. S., Goins, B., Timmons, J. H., Klipper, R. and Blumhardt, R. A simple method for producing a technetium-99m-labeled liposome which is stable in vivo. Nucl Med Biol 19: 539-547, 1992. Hernandez M. and Rosenthall, L. A cross-over study comparing the kinetics of Tc-99m-labeled isopropyl and p-butyl IDA analogs in patients. Clin Nucl Med 5:159-165, 1980. Klingersmith, W. C., Fritzberg, A. R. and Spitzer, V. M. Clinical comparison of Tc-99m diisopropyl-IDA and diethyl-IDA for evaluation of the hepatobiliary system. Radiology 140: 791-795, 1981. Allen, T. M., Hansen, C., Martin, F., Redemann, C. and Yau-Young, A. Liposomes containing synthetic lipid derivatives of poly (ethylene glycol) show prolonged circulation half-lives in vivo. Biochim Biophys Acta 1066: 29-36, 1991. Fiske, C. H. and Subbarow, Y. The colorimetric determination of phosphorus. J Biol Chem 66: 375-400, 1925. New, R. R. C. Paper chromatography of labeled liposomes, in New R.R.C. (ed) Liposomes: a practical approach, IRL Press, New York, NY, pp105-162, 1990. Wu, M. S., Robbins, J. C., Ponpipom, M. M. and Shen, T. Y. Modified in vivo behavior of liposomes containing synthetic glycolipids. Biochim Biophys Acta 674: 19-29, 1981. Gabizon, A., Price, D. C., Huberty, R. S. and Papahadjopoulos, D. Effect of liposome composition and other factors on the targeting of liposomes to experimental tumors: biodistribution and imaging studies. Cancer Res 50: 6371-6378, 1990. Goins, B., Klipper, R., Rudolph, A. S., Cliff, R. O., Blumhardt, R., and Phillips, W. T. Biodistribution and imaging studies of technetium-99m-labeled liposomes in rats with focal infection. J Nucl Med 34: 2160-2168, 1993. Espinola, I. R., Dunnick, J. K., Goris, M. L. and Kriss, J. P. Radiolabeled liposomes as metabolic and scanning tracers in mice. II. In-III oxime compared with Tc-99m-DTPA, entrapped in multilamellar lipid vesicles. J Nucl Med 20: 434-440, 1979. Love, W. G., Amos, N., Williams, B. D. and Kellaway, I. W. Effect of liposome surface charge on the stability of technetium (99mTc) radiolabelled liposomes. J Microencapsul 6: 105-113, 1989. Loberg M.D., Cooper, M. and Harvey, E. Development of new radiopharmaceuticals based on N-substitution of iminodiacetic acid. J Nucl Med 17: 633-638, 1976. Wistow, B. W., Subramanian, G. and Van Heertum, R. L. An evaluation of 99mTc-labeled hepatobiliary agents. J Nucl Med 18: 455-461, 1977. Cooper A. J. L. Biochemistry of sulfur-containing amino acid. Ann Rev Biochem 52: 187-222, 1983. Saha, G. B. Normal biodistribution of diagnostic radiopharmaceuticals, in Hladik, W. B., Saha, G. B. and Study, K. T. (eds) Essentials of nuclear medicine science, Williams and Wilkins, Baltimore, MD, pp3-19, 1987. Allen, T. M. Long-circulating (sterically stabilized) liposomes for targeted drug delivery. Trends in Pharmacol Sci 15: 215-220, 1994. Woodle, M. C. and Lasic D. D Sterically stabilized liposomes. Biochim Biophys Acta 1113: 171-199, 1992. Allen, T. M., Mehra, T., Hansen, C. and Chin, Y. C. Stealth liposomes: an improved sustained release system for 1-beta-D-arabinofuranosylcytosine. Cancer Res 52: 2431-2439, 1992. Woodle, M. C. Gallium-67-labeled liposomes with prolonged circulation: preparation and potential as nuclear imaging agents. Nucl Med Biol 20: 149-155, 1993. Corresponding author: Mavanur R. Suresh, Faculty of Pharmacy and Pharmaceutical Sciences, University of Alberta, Edmonton, Alberta, Canada. T6G 2N8
Published by the Canadian Society for Pharmaceutical Sciences. Copyright © 1997 by the Canadian Society for Pharmaceutical Sciences. |